Авторы: , , Кучур П.Д.,, Анна Штро
Abstract
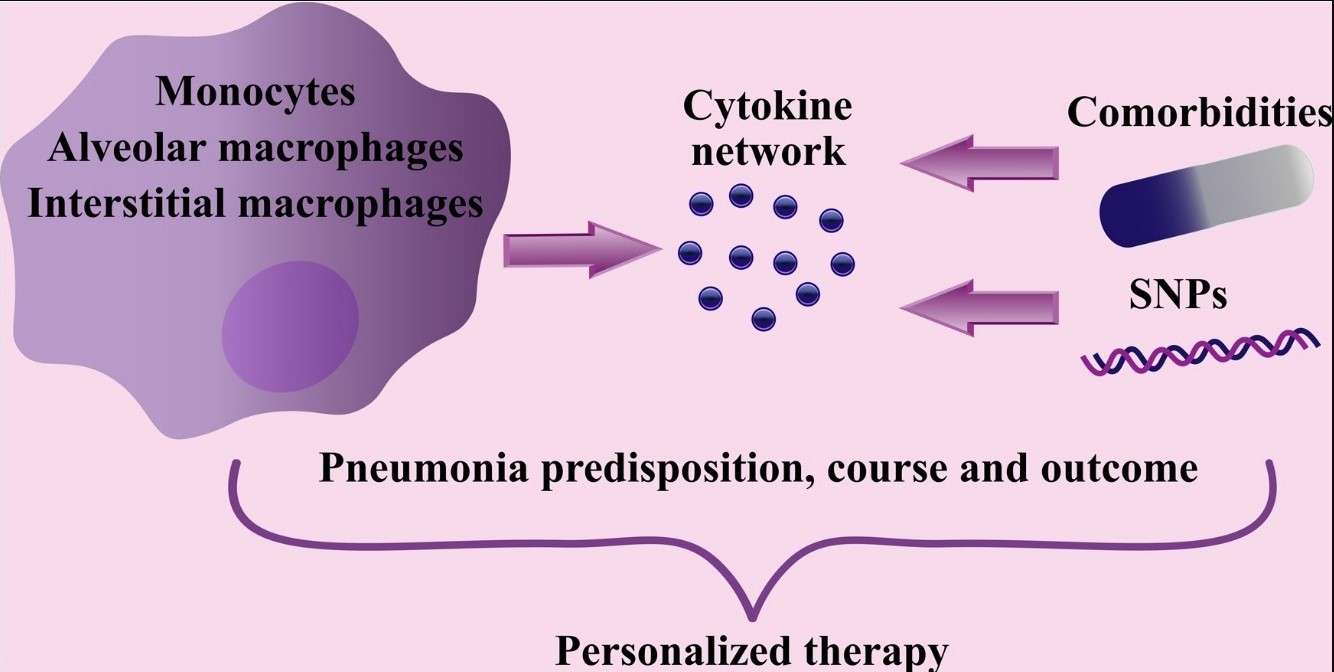
Macrophages represent the first line of anti-pathogen defense - they encounter invading pathogens to perform the phagocytic activity, to deliver the plethora of pro- and anti-inflammatory cytokines, and to shape the tissue microenvironment. Throughout pneumonia course, alveolar macrophages and infiltrated blood monocytes produce increasing cytokine amounts, which activates the antiviral/antibacterial immunity but can also provoke the risk of the so-called cytokine “storm” and normal tissue damage. Subsequently, the question of how the cytokine spectrum is shaped and balanced in the pneumonia context remains a hot topic in medical immunology, particularly in the COVID19 pandemic era. The diversity in cytokine profiles, involved in pneumonia pathogenesis, is determined by the variations in cytokine-receptor interactions, which may lead to severe cytokine storm and functional decline of particular tissues and organs, for example, cardiovascular and respiratory systems. Cytokines and their receptors form unique profiles in individual patients, depending on the (a) microenvironmental context (comorbidities and associated treatment), (b) lung monocyte heterogeneity, and (c) genetic variations. These multidisciplinary strategies can be proactively considered beforehand and during the pneumonia course and potentially allow the new age of personalized immunotherapy.
Read full: https://www.sciencedirect.com/science/article/pii/S135961012030229X